Regardless of epidermal closure type, deep suture placement was used in an average (standard deviation ) of 88.8% (19.5%) of cases overall, which did not statistically differ between years of Mohs experience or practice setting (Table 2). The average age of respondents was 45 years 69.1% (n =47) of respondents were male, and 76.5% (n =52) practiced in a private setting (Table 1). Sixty-eight ACMS fellowship-trained Mohs surgeons completed the survey. Statistical significance was determined as P <.05. Comparisons were made between practice habits, preferences, and surgeon demographics using t tests. Respondents indicated their frequency of using deep sutures, epidermal sutures, and wound undermining on a sliding scale of 0% to 100%. Surgeons were asked about their preferred method for scalp wound closure as well as clinical and economic variables that impacted those preferences. The 10-question survey was approved by the University of Kansas institutional review board and the executive committee of the ACMS. Frequent dressing change is recommended to reduce the risk of infection, while allowing exposure to air to help the wound heal faster.The Evolution of the Micrographic Surgery and Dermatologic Oncology Fellowship MethodsĪn anonymous survey was distributed from April 2019 to June 2019 to fellowship-trained Mohs surgeons using an electronic mailing list from the American College of Mohs Surgery (ACMS). Finally, the patient's wound should be closely monitored to prevent dehiscence from reccurring.

Next the wound must be closed properly with the appropriate surgical technique and sutures. Surgical debridement is typically performed to treat wound dehiscence by removing the dead or infected tissue to enable better healing of the wound. Antibiotics may be used to prevent any future infections if none were present, as woundĭehiscence increases the risk of wound infection. The antibiotic therapy used to treat the patient is considered, along with any ongoing infection that might have caused the dehiscence. A wound dehiscence is treated as a new wound, and takes into consideration the surgical history of the wound.
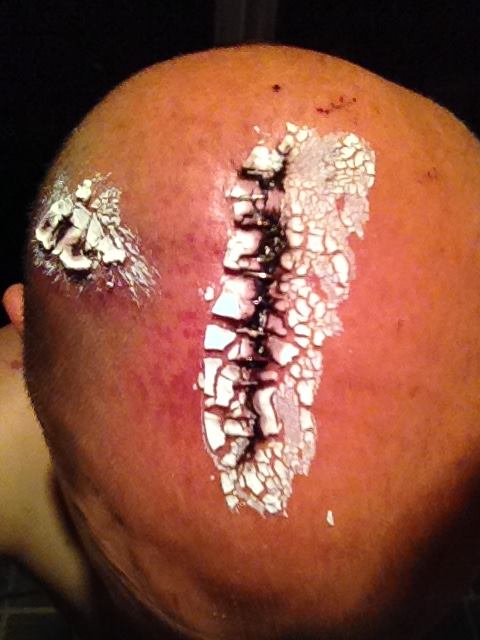
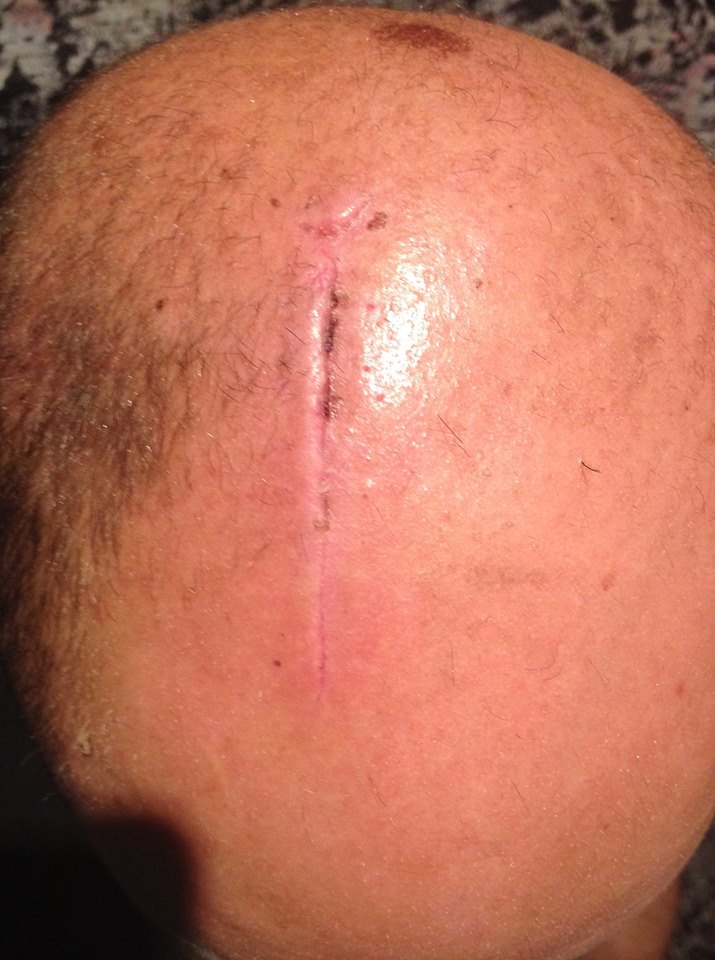
In some cases, wound dehiscence could be secondary to wound infection or poor healing as seen in patients with chronic diseases, malnutrition or weak immune systems. Wound dehiscence can also be caused by increased stress to the wound area as a result of strenuous exercise, heavy lifting, coughing, laughing, sneezing, vomiting or bearing down too hard with bowel movement. Wound dehiscence can be caused by poor surgical techniques such as improper suturing, over-tightened sutures or inappropriate type of sutures. However, when wound dehiscence occurs, the edges starts to separate and the wound reopens instead of healing closed as planned.

Typically, the sutures or closures around wound edges should stay intact while new tissue, known as "granulation tissue," starts forming to help heal the wound. Wound dehiscence is one of the most common complications of surgical wounds, involving the breaking open of the surgical incision along the suture.
